"Uncover the truth behind the groundbreaking discovery of the causes of the world's biggest problems. 'The Root Causes' will change how you view the world!"
Understanding the Causes of Arterial Plaque Buildup
Arterial plaque buildup is a significant factor in the development of atherosclerosis, a condition that leads to cardiovascular damage and increases the risk of heart attacks and strokes. While traditional treatments like statins and PCSK9 inhibitors are commonly used as cholesterol-lowering medications, recent research highlights the potential of anti-inflammatory drugs in reducing arterial plaque and potentially shrinking arterial plaque size. These therapies focus on targeting inflammation, which plays a key role in plaque formation and rupture, offering an alternative approach to heart disease prevention and atherosclerosis reversal. By utilizing anti-inflammatory therapy for atherosclerosis, patients may experience better management of heart health and plaque reduction, without solely relying on cholesterol-lowering medications. The goal is to stabilize plaques, prevent further cardiovascular damage, and support long-term heart health.
DISEASESNUTRITION
Glenn Rosaroso Vale, BSMT, MS(IT), MBA
12/3/20243 min read
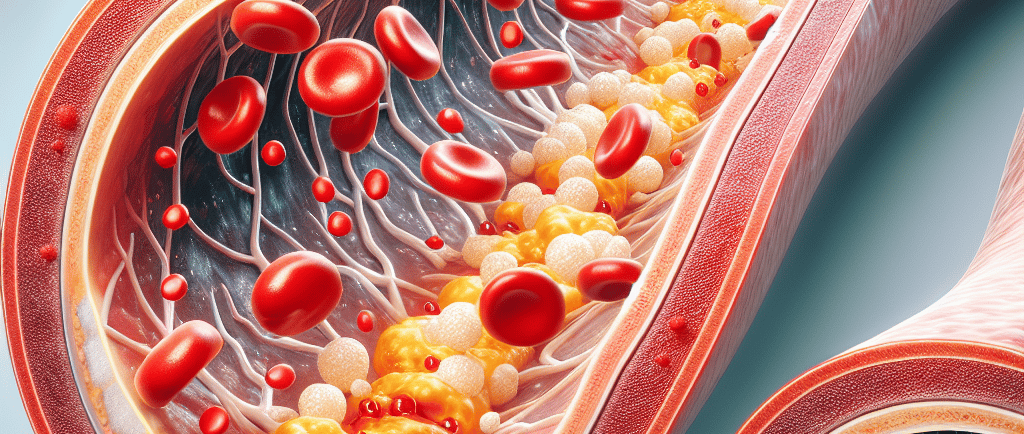
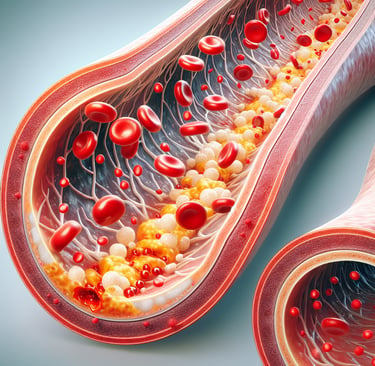
What is Arterial Plaque?
Arterial plaque is a critical health concern that occurs when fatty deposits, small dense atherogenic cholesterol, and other substances accumulate in the walls of arteries. This buildup, which leads to a condition called atherosclerosis, can have severe consequences for cardiovascular health. Over time, plaque hardens and narrows the arteries, restricting blood flow to vital organs such as the heart and brain. As the condition progresses, it significantly increases the risk of serious health events like heart attacks and strokes, making it essential to understand how arterial plaque forms and the steps we can take to prevent or manage its development.
How Does Arterial Plaque Form?
The formation of arterial plaque begins with damage to the inner lining of the arteries. This damage often results from factors such as high blood pressure, high small dense and oxidized LDL- cholesterol, smoking, and diabetes. One of the key contributors to arterial plaque formation is hypertension, which increases pressure against the endothelial walls of arteries. This heightened pressure damages the protective layer of the artery, known as the glycocalyx, leading to a reduction in nitric oxide production. Nitric oxide plays a crucial role in helping blood vessels relax and dilate, and without it, vasoconstriction occurs, causing blood vessels to narrow further.
The narrowing of blood vessels due to vasoconstriction contributes to an increase in blood pressure, exacerbating the damage to the artery walls. This cycle makes it easier for fatty deposits, particularly small dense LDL cholesterol, to infiltrate the damaged areas, leading to the development of plaque.
Lifestyle factors, particularly diet, play a major role in the development of arterial plaque. A diet high in carbohydrates, processed, and seed oils triggers inflammation in the endothelial cells, which further promotes plaque buildup. Smoking also damages the blood vessels, while diabetes contributes to increased glucose levels that damage artery walls.
The Risk of Plaque Build-Up
As the plaque accumulates and hardens over time, the affected arteries become less flexible and narrowed. This condition, known as atherosclerosis, impedes blood flow, making it more difficult for oxygen and nutrients to reach vital organs. Eventually, the plaque may rupture, leading to the formation of a blood clot, which can completely block the artery. If this occurs in the heart, it results in a heart attack; if it happens in the brain, it can cause a stroke.
Prevention and Management
Preventing and managing arterial plaque involves addressing the root causes of plaque formation. Here are some key strategies:
Dietary Changes: A diet contains low glycemic fruits, vegetables, whole grains (limit to 4 grams only per meal), and healthy fats (such as omega-3 fatty acids) can help lower small dense LDL- cholesterol levels and reduce inflammation. Reducing processed carbohydrates, sugar and seed oil intake is also crucial for maintaining a healthy endothelial lining.
Exercise: Regular physical activity, including high-intensity interval training (HIIT), can improve heart health, lower small dense LDL-cholesterol, and enhance blood vessel function by promoting nitric oxide production.
Blood Pressure Control: Monitoring and managing blood pressure through lifestyle changes, such as reducing salt intake and managing stress, is essential for preventing artery damage.
Weight Management: Maintaining a healthy weight can lower the risk of high cholesterol, hypertension, and diabetes, all of which contribute to plaque formation.
Medications: Although statins and PCSK9 inhibitors are typically used to lower cholesterol, recent research is emphasizing the potential of anti-inflammatory drugs in slowing plaque progression and potentially shrinking arterial plaque. Inflammation plays a crucial role in both the formation and rupture of plaques, so targeting inflammation with specific therapies could help stabilize these plaques and prevent additional cardiovascular damage. By focusing on reducing inflammation, these treatments aim to support heart disease prevention and may contribute to atherosclerosis reversal, all without the need for traditional cholesterol-lowering medications.
Conclusion
Arterial plaque is a serious medical condition that can lead to dangerous cardiovascular diseases like heart attacks and strokes. Its formation is often linked to unhealthy lifestyle habits, including poor diet, lack of exercise, smoking, and unmanaged blood pressure. By making proactive changes in diet, exercise, and overall health, we can reduce the risk of plaque buildup and improve heart health. Early intervention and lifestyle adjustments are essential for maintaining healthy arteries and preventing the progression of atherosclerosis.
Health
Understanding illness to empower your well-being journey.
Wellness
Knowledge
info@rootcauseprevention.com
903-268-6664
© 2024. All rights reserved.
grfv@sbcgloal.net